It’s a common albeit misguided belief that people with vaginas have a higher threshold for pain, thanks to an evolutionary history of childbirth. But we know that having a vagina certainly doesn’t make pain any less, well, painful (or real)—especially when our vaginas are the source of pain. In fact, researchers found that vulva owners actually tend to feel pain more intensely, particularly when it comes to acute and chronic inflammation.
The pervasive idea that having a vagina (somehow, some way?) lessens physical pain highlights our cultural confusion between pain threshold and pain tolerance and often invalidates uterus-owners’ pain altogether, brushing off debilitating body-wide pain or inflammation as “bad PMS.”
To clarify, pain threshold is the point at which a person initially starts to sense pain once exposed to a stimulus (like a hot stove, the corner of your coffee table, or an infected ingrown hair). Pain tolerance, however, refers to the amount of pain one can handle without doubling over in agony. In other words, the stimuli can be measured, but the experience of pain remains entirely subjective. It’s worth repeating that everybody and every body is different, and there are several factors that affect the way someone experiences—and deals with—pain.
Unfortunately, the medical industry has a long history of excluding people with vulvas from their research, which has lent a hand in misdiagnosing and under-diagnosing chronic pelvic pain among uterus-owners. If we’ve learned anything over the years, it’s that the symptoms of chronic pelvic pain are vast, yet the diagnosis and treatment options remain limited.
Take a hot Tonic bath to stimulate Blood flow and ease tension: Shop Tonic
Many people with chronic pelvic pain remain undiagnosed and are therefore untreated for years, leaving those affected feeling alone in their search for alternative solutions to heal and soothe their bodies. Oftentimes, people with chronic pelvic pain, prolonged or heavy periods, or painful cramps (to name just a few) will say they always knew something was wrong, but they didn’t feel heard, or that their pain was validated. That’s because these symptoms, while severe, are rarely taken seriously by doctors because there is an assumption that "periods are painful" anyway, so there’s no need to further investigate the cause(s) of these symptoms.
Chronic pain (excruciating or mild) is never normal and you don’t have to (and shouldn’t) suffer in silence.
We’re listening, and we’re here to discuss how chronic pelvic pain can manifest in the body, how to build a personal toolbox to manage symptoms, and how to be an advocate for these conditions while building a community for support. As always, questions, insights, and other resources are welcome!
Soothe vulvovaginal dryness, itching, and irritation: Shop Salve
Different Types of Chronic Pelvic Pain
Chronic pelvic pain affects 1 in 5 people with vulvas and 1 in 10 people with penises at some point in their lives. It is defined as persistent albeit noncyclic pain occurring anywhere related to the pelvis including the abdomen, pubic, perineum, and rectal areas and lasts more than six months. The cause for CPP can be gynaecological, urological, gastrointestinal, musculoskeletal, psychoneurological, and in most cases, it’s a combination.
Many symptoms and conditions play a role in developing chronic pelvic pain, so we’ve compiled a list of some of the most prevalent conditions below. Please note that this is by no means a comprehensive list, and we will be rolling out more pelvic health information throughout.
Pelvic Inflammatory Disease
An infection of the female-defined reproductive organs.
Pain Areas: pelvis, vagina, lower back
Inflammation Areas: ovaries, fallopian tubes, uterus
Other symptoms: fever, vaginal discharge, chills, cramping
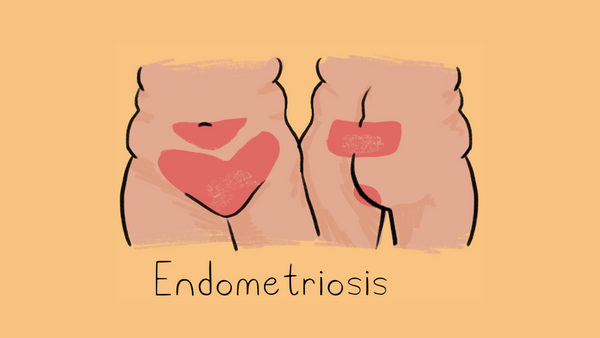
Endometriosis
A disorder in which tissue similar to the tissue that lines the uterus grows in other parts of your body. Learn more about endometriosis here.
Pain Areas: pelvis, lower abdomen, rectum, vagina, lower back
Inflammation Areas: ovaries, fallopian tubes, intestines
Other symptoms: abnormal menstruation, prolonged period, constipation, infertility, pain while defecating
*Endometriosis has been found throughout the body, and there are different types of endometriosis that affect different parts of the body, such as urinary endometriosis and thoracic endometriosis, which affects the lungs.
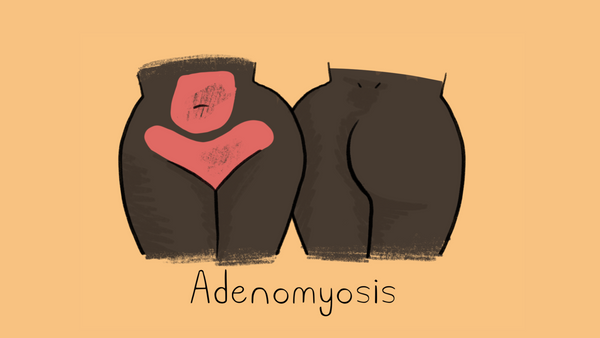
Adenomyosis
When tissue from the endometrium grows into the uterine wall, causing the uterus to swell. Learn more about adenomyoisis here.
Pain Areas: pelvis, abdomen
Inflammation Areas: uterine wall
Other symptoms: heavy menstruation, prolonged period, severe cramping, blood clot passed during menstruation
Ovarian Cyst
Solid or fluid filled sack in or on one's ovary.
Pain Areas: lower back, pelvis, abdominal side
Inflammation Areas: ovary / ovaries
Other symptoms: cramping, excessive hairiness *often symptomless
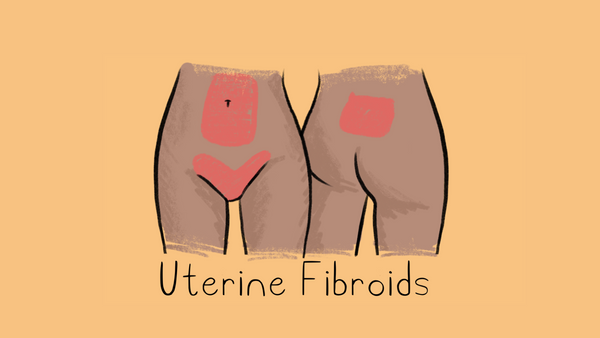
Uterine Fibroids
Growths In the uterus that are non-cancerous. Learn more about uterine fibroids here.
Pain Areas: abdomen, lower back, pelvis
Other symptoms: heavy menstruation, prolonged period
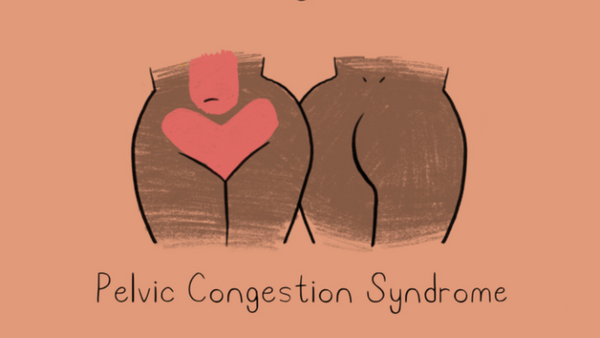
Pelvic Congestion Syndrome
Chronic pelvic pain caused by enlarged veins in the pelvic region. Learn more about pelvic congestion syndrome here.
Pain Areas: abdomen, lower back, pelvis.
Other symptoms: pain before or during periods, irritable bladder and/or bowels, pain during urination and/or sex, enlarged and distorted veins on the buttocks, vulva, or thighs
Other Pelvic Pain Conditions
Appendicitis When your appendix becomes inflamed, swollen, or infected. Pain often pain starts in the middle to lower abdomen and travels to your lower right-hand side
Mittelschmerz Ovulation pain. Can be dull, sharp, or cramp-like. Usually one sided and felt in the lower abdomen.
Urinary Tract Infection When any part of one’s urinary system is infected including the urethra or bladder. Symptoms include pelvic and/or abdominal pain.
Interstitial Cystitis Also called painful bladder syndrome; IC causes bladder pressure and pelvic pain. It’s causes remain unknown.
Pelvic Organ Prolapse When an organ in one’s pelvis like the uterus or bladder drops from its normal position. A prolapse often happens after pregnancy or during or after menopause.
Urinary Stones/ Bladder Stones When the minerals in one’s urine crystalize and become masses because one cannot fully empty their bladder.
Pelvic Adhesions After a surgery, pelvic infection, or endometriosis, bands of scar tissue can cause organs in the pelvic region to stick together
Advocate For Your Health
If you experience any of these symptoms, or are concerned you have one of the chronic pelvic pain conditions above, schedule an appointment with your doctor as soon as possible. Anytime something feels “off," it’s worth looking into—especially when you’re experiencing pain for a prolonged period of time, or it begins to interfere with your daily life.
In addition to tracking your pain, bleeding, and other physical symptoms, pay attention to other circumstances that could be contributing to these side effects, like your diet, sleep schedule, stress levels, or type of birth control so that you can have a comprehensive discussion with your doctor about your concerns to find the root of the problem, rather than short term solutions.
Beyond a visual inspection, some other diagnostic tests you can ask for include:
- An ultrasound
- MRI scans
- CA125
- Laparoscopy (can be used to diagnose and treat)
If you feel your doctor is not giving you the information you need to feel confident in your diagnosis, don’t be afraid to ask for a second opinion, and do your own research as well. The only real way to end the myth that chronic pelvic pain symptoms are “normal” or "just period cramps" is to challenge the way things are done in the medical community. Don't be afraid to ask for more research, more tests, and more answers. It’s likely going to be a long and frustrating process but you—and your reproductive health—are worth it.
Resources for Chronic Pelvic Pain
The Happy Pelvis
Regardless of which condition(s) affect you, chronic pelvic pain has a significant impact on quality of life. Michelle of @the.happy.pelvis is a Canadian based chronic pelvic pain sufferer who has chronicled her journey to raise awareness about chronic pelvic pain and support others struggling just like her. Follow her journey and learn more here.
Qendo
Quendo is dedicated to supporting anyone affected by endometriosis, adenomyosis, PCOS or infertility through education, support and awareness. They provide a free membership offering resources to help educate and build your toolkit to manage CPP while their app helps you track symptoms. They even offer a 24/7 support line available for people to use all over the world. Learn more here. Follow QENDO at @qendoau.
The Endo Co
The Endometriosis Coalition is a non-profit organization that supports and empowers the lives of those living with endometriosis. They aim to raise awareness, promote reliable education, and increase research funding for Endometriosis, Adenomyosis, and other chronic pelvic pain conditions. Learn more here and follow them @theendo.co.
Further Reading
Understanding Uterine Fibroids
Endometriosis with Venus Libido
Learn What Your Period Blood Is Telling You About Your Health
Decode Your Vaginal Discharge
Learn How Each Phase of the Menstrual Cycle Affects Your Immunity
Momotaro Apotheca and its materials are not intended to treat, diagnose, cure or prevent any disease. All material on Momotaro Apotheca is provided for educational purposes only. Always seek the advice of your physician or another qualified healthcare provider for any questions you have regarding a medical condition.